Insurance Department Recovers $6 Million for Policyholders, Taxpayers in 2015; Recoveries, Fines Both At 4-Year Low
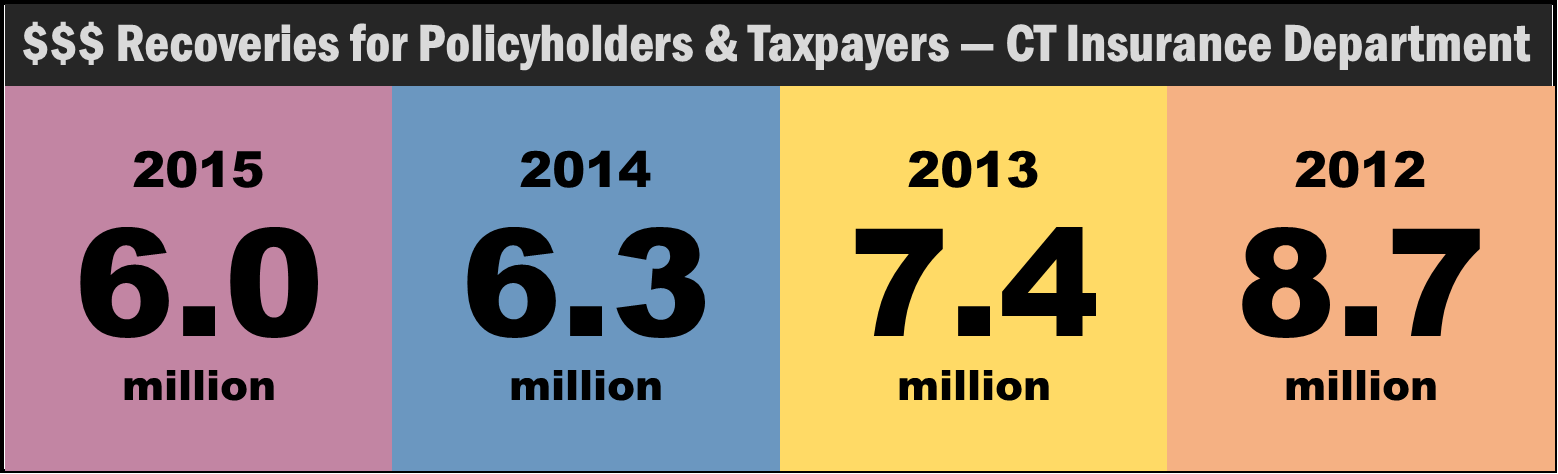
/The Connecticut Insurance Department recovered approximately $6 million for policyholders and taxpayers in 2015, helping individuals and families with their claims and complaints. The total dollar amount of the recoveries declined for the third consecutive year, down from a high of $8.7 million in 2012, $7.4 million in 2013 and $6.3 million in 2014.
Officials indicated that the Department’s Consumer Affairs Unit (CAU) fielded more than 6,100 complaints and inquiries and helped policyholders recoup more than $4 million from January 1 to December 31, 2015. The number of complaints and inquiries dropped slightly from the previous year, when 6,500 were handled, recouping $4.3 million for policy owners. In 2013, policyholders saw $4.7 million returned. In 2012, the numbers were virtually identical to 2015.
“Behind these statistics are the individuals and families the Department was able to help through our intervention,” Commissioner Katharine L. Wade said. “In many cases we were able to make a real difference in their lives and I encourage anyone with questions or concerns about their insurance to contact the Department. We are here to help consumers.”
The department, in announcing the annual totals for 2015, also highlighted some individual recoveries, including:
- $27,000 for home health care services for a senior citizen under her long-term care policy
- $13,000 to pay for speech therapy for an autistic child
- $16,000 paid to a policyholder for an inpatient stay at a skilled nursing facility
- $37,000 in an additional payment to a homeowner to settle a claim
“Our staff makes certain that companies and agents comply with all state insurance laws and regulation and have extensive knowledge to answer a wide range of insurance questions,” the Commissioner said.
In addition to recoveries for policyholders, the Department’s Market Conduct division levied approximately $1.7 million in fines against carriers and returned that money to the state General Fund in 2015. The fines resulted from a variety of violations and settlements ranging from untimely claim payments to improper licensing. That was the lowest total for fines in recent years, perhaps signifying greater compliance. In 2014, fines totaled $2.03 million, in 2013 the total was $2.7 million and in 2012 fines levied totaled $4.6 million.
The majority of the funds recovered for policyholders stemmed from complaints over health, accident, homeowners and life and annuities policies.
The following is the breakdown of funds recovered in 2015:
- Accident, Health - $2.7 million, compared with $2.5 million in 2014
- Auto - $430,000, compared with $381,000 in 2014
- General Liability - $17,200, compared with $65,000 in 2014
- Homeowners - $530,000, compared with $65,000 in 2014
- Life, Annuities - $294,000, compared with $330,000 in 2014
Recoveries in 2013 were largely focused on homeowners, as a result of Superstorm Sandy-related claims. Department recoveries in 2012 reflect the impact of claims from 2011 Storm Irene and the late October snow-filled Nor’easter that landed in Connecticut.
The Department calculates its consumer recoveries based on what the policyholder received as a result of the Department’s intervention. The inquiries and complaints also help the Department identify industry trends that may adversely affect consumers and trigger investigation by the Market Conduct division, officials said.
In addition, complaint data also help determine topics for consumer education and serve as tools to help the Department monitor the industry. The Market Conduct enforcement actions are posted on the Department’s web site at www.ct.gov/cid